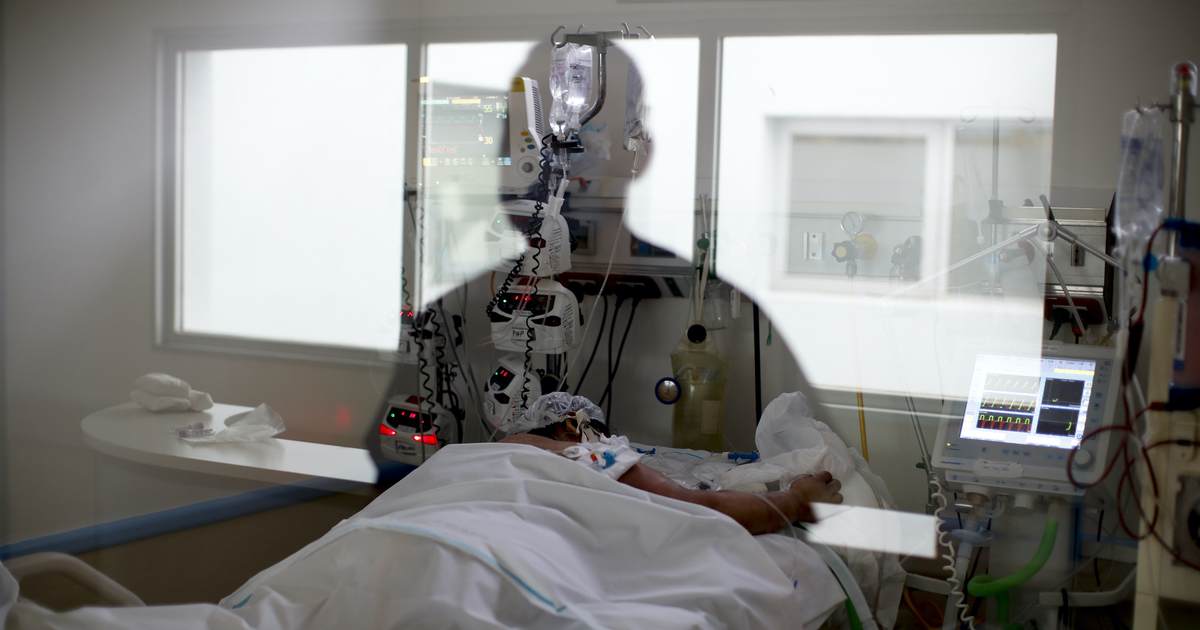
Kameron Gilchrist was accused of removing his IV at UNC Rex Hospital in Raleigh and spraying medical staff with his HIV-positive blood; the legal outcome that followed was a short sentence and credit for time already served.
The incident unfolded while Gilchrist was being treated for a diabetic episode at the hospital last March, according to the account in the arrest documents. Staff say he pulled out his IV and directed his blood toward hospital workers, who were then treated as victims in the assault. The case later returned to public attention when authorities completed a criminal process that included psychiatric and medical holds.
An arrest warrant describes the act plainly and notes the patient’s HIV-positive status. The reported timeline shows the event happened on March 21, 2025, but Gilchrist was not arrested until months later because he remained under medical and psychiatric care. That delay affected how the case moved forward and factored into later decisions about detention and prosecution.
A hospital patient allegedly removed an IV from his arm and used his “HIV positive blood” as a weapon by spraying it into the eyes of medical personnel.
According to an arrest warrant obtained by Law&Crime, 25-year-old Kameron Gilchrist was being treated for diabetes at UNC Rex Hospital on March 21, 2025.
Gilchrist began spraying “his HIV positive blood at the victims’ eyes” by “removing his IV from his arm,” per the warrant. It was not made clear if the victims, both hospital employees, contracted HIV.
Gilchrist was not arrested until September because he was still receiving medical and psychiatric treatment at the time of the incident and could not immediately be arrested, per local outlet WRAL.
Under North Carolina law, assaulting health-care personnel is a serious offense, classified as a Class I felony at the baseline, with higher charges available when weapons or severe injury are involved. Class I felonies carry a maximum prison term of 24 months, but different charges and facts can elevate exposure to longer terms. In this case prosecutors pursued a charge of assault with a deadly weapon, which can carry a sentence of up to seven years when aggravated by particular facts.
When the case reached resolution, Gilchrist accepted a plea deal that produced a much shorter punishment than the upper range of potential exposure. The judgment recorded a 91-day sentence and contemporaneous credit for 91 days of time he had already spent in custody. That calculation effectively left him without additional jail time after the plea was entered and the credit applied.
That 91-day sentence reflects the bargain struck in the plea rather than the full statutory maximum for the aggravated charge. Prosecutors sometimes negotiate reduced terms when there are complicating medical or mental health issues, victims are cooperative with a plea, or other practical considerations influence the case timeline. The result in this instance meant the defendant avoided a multi-year prison term that the harsher charge could have carried.
Questions follow when a violent act targets medical staff, who are obligated to provide care and cannot refuse treatment to someone in need. Hospitals and clinicians must balance patient rights, duty to treat, and staff safety; the legal system is where the consequences for violent acts are meant to be enforced. Observers and affected staff often contend that outcomes like short sentences weaken the deterrent effect against assaults on health-care workers.
🛑NORTH CAROLINA MAN WEAPONIZES HIS HIV POSITIVE BLOOD AGAINST HOSPITAL STAFF AND WALKS FREE IMMEDIATELY
A 25-year-old man named Kameron Gilchrist intentionally attacked two hospital workers at UNC Rex Hospital in Raleigh North Carolina. While they were treating him for diabetic… pic.twitter.com/8YvTd7sXVo
— @XTexasGirlX (@XtexasgirlX) March 30, 2026
The hospital addressed the incident publicly and expressed concern for staff safety in the wake of the event. A spokesperson for UNC Rex said, “Unfortunately, violent situations and threats of violence against health workers have become more common across the country.” That comment echoed a broader trend hospitals report: increasing frequency of aggressive encounters involving patients or visitors in care settings.
From the criminal justice side, the interplay between medical treatment, psychiatric evaluation, and prosecution is often complex. Delays in arrest while a defendant remains in medical or psychiatric care can change charging decisions and bargaining positions. Defendants with overlapping health needs may face different pathways through court than those who are immediately detained and tried.
For hospital staff and administrators, the case raises practical questions about workplace protections and how institutions and prosecutors coordinate when employees are targeted. It also highlights the tension between ensuring patient access to care and maintaining a safe environment for clinicians. Incidents like this prompt renewed attention on prevention, training, and legal remedies for violent acts in clinical settings.